Transitional Program Office to Advance Graduate Medical Education in California
In April 2020, Mathematica established a two-year Transitional GME Program Office to advance GME expansion in California. The Transitional Program Office provides interim leadership related to GME expansion in California; coordinating with GME experts and leaders at the state and national levels and producing resources such as toolkits for health care organizations interested in developing or expanding GME programs.
The Transitional Program Office is guided by an advisory board of GME experts from a variety of training hospitals and Teaching Health Centers representing different California geographic regions, health systems, disciplines, and medical specialties.
Grant Funding for GME Naïve Hospitals
Mathematica is working with philanthropic foundations to accelerate GME expansion efforts across California. As part of this work, we oversee a small grant program for non-teaching hospitals interested in exploring the feasibility of starting GME programs. In February 2021, five grants were awarded to hospitals located throughout the state (as shown in the map below). In September 2021, we announced additional awards for two feasibility grants and two start up grants.
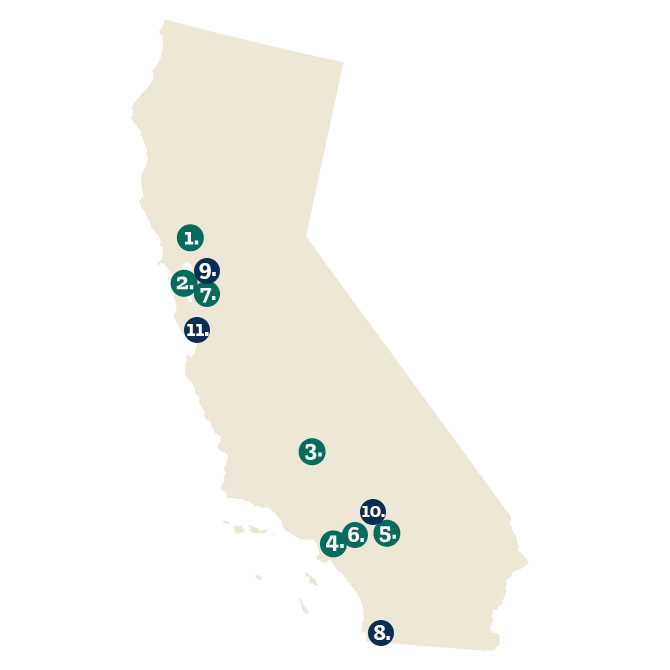
Funded Proposals (February 2021)
- Adventist Health Saint Helena (St. Helena, CA)
- Chinese Hospital (San Francisco, CA)
- Good Samaritan Hospital (Oildale, CA)
- St. Francis Medical Center (Lynwood, CA)
- Mountains Community Hospital (Lake Arrowhead, CA)
Additional Approved Proposals (February 2021)
- Aurora Charter Oak Hospital (Covina, CA)
- Stanford Health Care – ValleyCare (Pleasanton, CA)
Funded Proposals (September 2021)
- Sharp Chula Vista Medical Center (San Diego, CA)
- Stanford ValleyCare (Pleasanton, CA)
- Desert Valley Hospital (Victorville, CA)
- Dominican Hospital (Santa Cruz, CA)
GME Resources Toolkit
Our team developed a toolkit of resources for GME expansion in California.
Health Issue Brief
Download briefCase Study of St. Joseph’s Medical Center
Download case studyWhy you should start a graduate medical education program at your hospital
Download presentationCase Study of Kaweah Delta Medical Center
Download case studyCase Study of John Muir Health
Download case studyCalifornia Health Care Foundation Issue Brief
Download resourceCalifornia Health Care Foundation Guide
Download resourceCalifornia Health Care Foundation Guide
Download resourceCalifornia Health Care Foundation Issue Brief
Download resourceCalifornia Health Care Foundation Issue Brief
Download resourcePublished Literature on GME Expansion
This study examined family medicine residencies to determine the costs and revenue per resident during the study period. The study found that overall expenses increased more than 70 percent from 2002 to 2014, and the median cost per resident increased 93.7 percent to $179,353. The study also found that total revenue per resident increased by only 44.5 percent from 2006 to 2016. The analysis showed that by 2016, there was a $47,164 difference between the median cost to train a resident and the revenue they brought to the institution. The researchers concluded that the excess expenses must be made up by other funding sources to ensure the viability of these family medicine residency programs.
Pauwels, J., and A. Weidner. “The Cost of Family Medicine Residency Training: Impacts of Federal and State Funding.” Family Medicine, vol. 50, no. 2, 2018, pp. 123–127. Available at https://www.ncbi.nlm.nih.gov/pubmed/29432627. Accessed May 27, 2020.
Because of the discrepancy between the geographic distribution of GME training programs and the needs of the U.S. population, along with other limitations of GME training programs, the Institute of Medicine convened a Committee on the Governance and Financing of GME in 2014. This article describes the purpose of the committee, the committee’s overarching goals for the future configuration of GME financing and governance, and the committee’s recommendation for distribution of GME funding.
Wilensky, G.R., and D.M. Berwick. “Reforming the Financing and Governance of GME,” New England Journal of Medicine, vol. 371, no. 9, August 18, 2014, pp. 792–793. Available at https://www.nejm.org/doi/full/10.1056/NEJMp1406174. Accessed May 27, 2020.
This article examines the benefits of residency programs in five areas: residents/fellows, institutions, local communities, university sponsors and affiliates, and the greater community/nation. The study found that the benefits of a residency program extend far beyond the training location and that the review of a residency program based solely on direct profits and losses might be insufficient. The authors argue that it is best to take into account direct and indirect revenue and expenses—with care given to examine the value of care given to poor and vulnerable populations—of the residency program as well as the intangible benefits of having a residency program (compared with the intangible benefits of other hospital-sponsored programs) when determining the financial sustainability of a residency program.
Pugno, P., W.R. Gillanders, and S.M. Kozakowski. “The Direct, Indirect, and Intangible Benefits of Graduate Medical Education Programs to their Sponsoring Institutions and Communities.” Journal of Graduate Medical Education, vol. 2, no. 2, June 2010, pp. 154–159. Available at https://www.jgme.org/doi/full/10.4300/JGME-D-09-00008.1. Accessed May 27, 2020.
Heilbrun, M.E., B. Poss, L. Boi, Y. Anzai, N. Hu, and R.S. Kaplan. “Assessing the Training Costs and Work of Diagnostic Radiology Residents Using Key Performance Indicators - An Observational Study.” Academic Radiology, vol. 27, no. 7, 2020, pp. 1025–1032. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7048663/. Accessed March 8, 2022.
Medvecz, A.J., T.J. Vogus, and K.P. Terhune. “The Cost of Not Training a Surgical Resident.” Journal of Surgical Education, vol. 78, no. 5, 2021, pp. 1443–1449. Available at https://pubmed.ncbi.nlm.nih.gov/33744117/. Accessed March 8, 2022.
Dewan, M.J., and J.J. Norcini. “We Must Graduate Physicians, Not Doctors.” Academic Medicine, vol. 95, no. 3, 2020, pp. 336–339. Available at https://journals.lww.com/academicmedicine/Fulltext/2020/03000/We_Must_Graduate_Physicians,_Not_Doctors.15.aspx. Accessed March 8, 2022.
He, K., E. Whang, and G. Kristo. “Graduate Medical Education Funding Mechanisms, Challenges, and Solutions: A Narrative Review.” American Journal of Surgery, vol. 221, no. 1, 2021, pp. 65–71. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7308777/. Accessed March 8, 2022.
Lauer, C.I., M. Shabahang, D. Hendricks, K. Mundy, S. Hayek, and E. Ryer. “Expansion of Surgical Graduate Medical Education Training Programs: A Return on Investment Analysis.” Journal of Surgical Research, vol. 258, 2021, pp. 278–282. Available at https://www.sciencedirect.com/science/article/pii/S0022480420306624. Accessed March 8, 2022.
Grischkan, J.A., A.B. Friedman, and A. Chandra. “Moving the Financing of Graduate Medical Education Into the 21st Century.” Journal of the American Medical Association, vol. 324, no. 11 2020, pp. 1035–1036. Available at https://jamanetwork.com/journals/jama/fullarticle/2770076.
Rittenhouse, D.R., A.S. Ament, and K. Grumbach. “Sponsoring Institution Interests, Not National Plans, Shape Physician Workforce in the United States.” Family Medicine, vol. 52, no. 8, 2020, pp. 551–556. Available at https://journals.stfm.org/familymedicine/2020/september/rittenhouse-2020-0088/.
Aizenberg, D.J., and L.S. Logio. “The Graduate Medical Education (GME) Gold Rush: GME Slots and Funding as a Financial Asset.” Academic Medicine, vol. 95, no. 4, April 2020, pp. 503–505. Available at https://journals.lww.com/academicmedicine/Fulltext/2020/04000/The_Graduate_Medical_Education__GME__Gold_Rush_.13.aspx?context=FeaturedArticles&collectionId=8.
Ashkin, E., W. Newton, B. Toomey, R. Lingley, and C. Page. “Cost of Incremental Expansion of an Existing Family Medicine Residency Program.” Society of Teachers of Family Medicine, vol. 49, no. 7, 2017, pp. 544–547. Available at https://www.stfm.org/FamilyMedicine/Vol49Issue7/Ashkin544. Accessed May 27, 2020.
Regenstein, M., K. Nocella, M.M. Jewers, and F. Mullan. “The Cost of Residency Training in Teaching Health Centers.” The New England Journal of Medicine, vol. 375, no. 7, August 18, 2016, pp. 612–614. Available at https://www.nejm.org/doi/10.1056/NEJMp1607866. Accessed May 27, 2020.
Savoj, J., C. Mikhail, R. Gulati, N. Ayutyanont, and A. Popa. “New Internal Medicine Residency Program at a Community Hospital Improves Mortality Without Increasing the Cost or Length of Stay: A Two-Year Follow Up.” Hospital Medicine Annual Conference, 2019. Available at https://scholarlycommons.hcahealthcare.com/teaching-learning/1/. Accessed June 2, 2020.
DeMarco, D.M., R. Forster, T. Gakis, and R.W. Finberg. “Eliminating Residents Increases the Cost of Care.” Journal of Graduate Medical Education, vol. 9, no. 4, 2017, pp. 514–517. Available at https://www.jgme.org/doi/full/10.4300/JGME-D-16-00671.1. Accessed Jun 2, 2020.
Bready, L., and M.P. Luber. “Costs Associated with Residency Training.” Texas Medicine, vol. 112, no. 2, 2016, pp. 44–49. Available at https://www.texmed.org/template.aspx?id=35119. Accessed June 2, 2020.
Eden, J., D. Berwick, and G. Wilensky. Graduate Medical Education That Meets the Nation's Health Needs. Chicago, IL: National Academies Press, 2014: https://www.ncbi.nlm.nih.gov/books/NBK248027/. Accessed June 2, 2020.
Wynn, B. “Opening the ‘Black Box’ of GME Costs and Benefits: A Conceptual Model and a Call for Systematic Studies.” Journal of Graduate Medical Education, vol. 7, no. 1, March 2015, pp. 125–127. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4507905/pdf/i1949-8357-7-1-125.pdf. Accessed June 2, 2020.
Caverzagie, K.J., S.W. Lane, N. Sharma, J. Donnelly, J.R. Jaeger, H. Laird-Fick, J.P. Moriarty, et al. “Proposed Performance-Based Metrics for the Future Funding of Graduate Medical Education: Starting the Conversation.” Academic Medicine, vol. 93, no. 7, July 2018, pp. 1002–1013. Available at https://journals.lww.com/academicmedicine/Fulltext/2018/07000/Proposed_Performance_Based_Metrics_for_the_Future.20.aspx. Accessed June 2, 2020.
Garces de Marcilla, J., K. Abreu, L. Peterson, and S. Weinman. “Teaching Hospitals and FQHCs Can Partner to Alleviate Community Healthcare Provider Shortages and Reduce Training Costs.” FQHC.org Blog, 2017. Available at https://www.fqhc.org/blog/2017/4/27/unusual-hospital-fqhc-partnerships-address-payment-and-access-issues. Accessed June 2, 2020.
This article discusses California’s health workforce shortage and highlights lack of funding as a barrier to expanding graduate medical education (GME) and, ultimately, the physician workforce. It builds on the previous findings of the California Future Health Workforce Commission and explains the role of GME-naive hospitals in GME expansion. The authors identify the most pressing needs of GME-naive hospitals, including start-up funding and technical assistance. They also highlight examples of GME expansion in GME-naive hospitals in other states.
Rittenhouse, D.R., and A.S. Ament. “Expanding Graduate Medical Education in California: The Role of GME-Naive Hospitals.” CHCF Health Workforce Strategies for California Series. 2021. Available at https://www.chcf.org/wp-content/uploads/2021/06/WorkforceSeriesGMENaiveHospitals.pdf. Accessed March 8, 2022.
This article explores the impact of the Veterans Access, Choice, and Accountability Act of 2014, which provided funding to the Department of Veterans Affairs (VA), the second largest federal funder of GME. The funding was intended to establish 1,500 positions, expanding VA-funded positions by 15 percent. The study found that the act was successful, stating that “at the conclusion of fiscal year 2021, 1,490 positions had been authorized, and 21 of the 22 VA medical centers previously without GME activity had added residents or were planning to soon.” The authors highlight that the VA’s success expanding physician GME training might serve as a model to address other shortages in the health workforce.
Klink, K., A. Albanese, E. Pope, and K. Sanders. “Veterans Affairs Graduate Medical Education Expansion Addresses U.S. Physician Workforce Needs.” Academic Medicine, 2021. Available at https://journals.lww.com/academicmedicine/Abstract/9000/Veterans_Affairs_Graduate_Medical_Education.96440.aspx. Accessed March 8, 2022.
In this article, directors of a new internal medicine residency program describe and reflect on their experience developing the program. The article includes the timeline and the key steps they followed to develop the program. The authors also discuss lessons learned, including that new residency programs can offer opportunities for innovation and that organizational culture, which is complex, will affect implementation of a program.
Bush, R.W., R.F. LeBlond, and R.D. Ficalora. “Establishing the First Residency Program in a New Sponsoring Institution: Addressing Regional Physician Workforce Needs.” Journal of Graduate Medical Education, vol. 8, no. 5, December 2016, pp. 655–661. Available at https://www.jgme.org/doi/full/10.4300/JGME-D-15-00749.1. Accessed May 27, 2020.
This article outlines the steps taken by Baylor College of Medicine and The Children’s Hospital of San Antonio to set up a new pediatric residency program in 2014 and can serve as a guide for future programs. The article includes information about infrastructure-building, curriculum development, accreditation, marketing, and recruitment for a new program. The article provides practical, “nuts and bolts” advice for those interested in creating a new residency.
Barajaz M., and T. Turner. “Starting a New Residency Program: A Step-by-Step Guide for Institutions, Hospitals, and Program Directors.” Medical Education Online, vol. 21, no. 1, 2016. Available at 10.3402/meo.v21.32271. Accessed June 2, 2020.
Ahmed, H., and J.B. Carmody. “On the Looming Physician Shortage and Strategic Expansion of Graduate Medical Education.” Cureus, vol. 12, no. 7, 2020, e9216. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7430533/. Accessed March 8, 2022.
Lauer, C.I., M. Shabahang, D. Hendricks, K. Mundy, S. Hayek, and E. Ryer. “Expansion of Surgical Graduate Medical Education Training Programs: A Return on Investment Analysis.” Journal of Surgical Research, vol. 258, 2021, pp. 278–282. Available at https://www.sciencedirect.com/science/article/pii/S0022480420306624. Accessed March 8, 2022.
Albanese, A.P., E.T. Bope, K.M. Sanders, and M. Bowman. “The VA MISSION Act of 2018: A Potential Game Changer for Rural GME Expansion and Veteran Health Care.” Journal of Rural Health: Official Journal of the American Rural Health Association and the National Rural Health Care Association, vol. 36, no. 1, 2020, pp. 133–136. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6973037/.
Shalaby, M., S.M. Higgins, J. Ojeda, and P. O’Rourke. “Logistics of Establishing a New Internal Medicine-Primary Care Program.” In Primary Care Track Toolkit, Second Edition. Alexandria, VA: Alliance for Academic Internal Medicine, 2020. Available at http://higherlogicdownload.s3.amazonaws.com/IM/fecab58a-0e31-416b-8e56-46fc9eda5c37/UploadedImages/Documents/resources/Primary_Care_Toolkit_Second_Edition.pdf#page=10.
Brown, J., M. Hendricks, and D. David. “For-Profit Systems Embrace Graduate Medical Education to Meet Demand for Primary Care Physicians.” Becker’s Hospital Review, 2019. Available at https://www.beckershospitalreview.com/hospital-physician-relationships/for-profit-systems-embrace-graduate-medical-education-to-meet-demand-for-primary-care-physicians.html. Accessed June 2, 2020.
Ashkin, E., W. Newton, B. Toomey, R. Lingley, and C. Page. “Cost of Incremental Expansion of an Existing Family Medicine Residency Program.” Society of Teachers of Family Medicine, vol. 49, no. 7, 2017, pp. 544–547. Available at https://www.stfm.org/FamilyMedicine/Vol49Issue7/Ashkin544. Accessed May 27, 2020.
Rieselbach, R., P. Shin, G. Nycz, K. Pereira, N. Short, E. McConnell, and K. Schmader. “Mega Teaching Health Centers: A New Model to Power CHCs.” Health Affairs Blog, 2016. Available at https://www.healthaffairs.org/do/10.1377/hblog20161013.057067/full/. Accessed June 2, 2020.
American Society of Health-System Pharmacists. “Residency Building and Expansion Toolkit.” n.d. Available at https://www.nmhanet.org/files/PharmacistResidencyToolkit.pdf. Accessed June 2, 2020.
This article explores the impact of the Veterans Access, Choice, and Accountability Act of 2014, which provided funding to the Department of Veterans Affairs (VA), the second largest federal funder of GME. The funding was intended to establish 1,500 positions, expanding VA-funded positions by 15 percent. The study found that the act was successful, stating that “at the conclusion of fiscal year 2021, 1,490 positions had been authorized, and 21 of the 22 VA medical centers previously without GME activity had added residents or were planning to soon.” The authors highlight that the VA’s success expanding physician GME training might serve as a model to address other shortages in the health workforce.
Klink, K., A. Albanese, E. Pope, and K. Sanders. “Veterans Affairs Graduate Medical Education Expansion Addresses U.S. Physician Workforce Needs.” Academic Medicine, 2021. Available at https://journals.lww.com/academicmedicine/Abstract/9000/Veterans_Affairs_Graduate_Medical_Education.96440.aspx. Accessed March 8, 2022.
The American Medical Association Council on Legislation and the AMA Council on Medical Education are continuing their partnership focusing on viable ways to improve graduate medical education (GME) to ensure medical students have the opportunity to fulfill training requirements and become practicing doctors. Workforce experts continue to predict that the U.S. will face a significant physician shortage for both primary care and specialty physicians over the next 10+ years if training positions are not expanded.
To adequately address these concerns, this document seeks to provide background regarding the challenges faced by the current GME system. This document also outlines GME initiatives including those by the AMA, private entities, and federal and state government that we hope will inform future GME advocacy.
American Medical Association. “Compendium of Graduate Medical Education Initiatives Report.” Chicago, IL: American Medical Association, 2020. Available at https://www.ama-assn.org/system/files/2020-08/2020-gme-compendium-report.pdf. Accessed June 3, 2021.
This compendium, compiled by the American Medical Association, outlines current and prospective proposals for changing the way graduate medical education (GME) is funded in the United States. The first section, Current GME Initiatives, outlines positions on GME reform put forward by prominent medical and educational associations, including the Institute of Medicine, the American Medical Association, the Association of American Medical Colleges, and the American Academy of Family Physicians. The second section, Proposals for GME Reform, outlines potential opportunities, challenges, and questions associated with different approaches to GME reform, including an all-payer model, the grow-your-own approach, and Teaching Health Center and Primary Care Residency Expansion grants.
American Medical Association. “Compendium of Graduate Medical Education Initiatives.” Chicago, IL: American Medical Association, 2016. Available at https://www.ama-assn.org/system/files/2019-02/gme-compendium.pdf. Accessed May 27, 2020.
Because of the discrepancy between the geographic distribution of GME training programs and the needs of the U.S. population, along with other limitations of GME training programs, the Institute of Medicine convened a Committee on the Governance and Financing of GME in 2014. This article describes the purpose of the committee, the committee’s overarching goals for the future configuration of GME financing and governance, and the committee’s recommendation for distribution of GME funding.
Wilensky, G.R., and D.M. Berwick. “Reforming the Financing and Governance of GME,” New England Journal of Medicine, vol. 371, no. 9, August 18, 2014, pp. 792–793. Available at https://www.nejm.org/doi/full/10.1056/NEJMp1406174. Accessed May 27, 2020.
He, K., E. Whang, and G. Kristo. “Graduate Medical Education Funding Mechanisms, Challenges, and Solutions: A Narrative Review.” American Journal of Surgery, vol. 221, no. 1, 2021, pp. 65–71. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7308777/. Accessed March 8, 2022.
Grischkan, J.A., A.B. Friedman, and A. Chandra. “Moving the Financing of Graduate Medical Education Into the 21st Century.” Journal of the American Medical Association, vol. 324, no. 11 2020, pp. 1035–1036. Available at https://jamanetwork.com/journals/jama/fullarticle/2770076.
Chen, C., Y. Chung, and S. Petterson. “Changes and Variation in Medicare Graduate Medical Education Payments.” JAMA Internal Medicine, vol. 180, no. 1, 2019, pp. 148–150. Available at https://jamanetwork.com/journals/jamainternalmedicine/article-abstract/2752363. Accessed March 8, 2022.
Rittenhouse, D.R., A.S. Ament, and K. Grumbach. “Sponsoring Institution Interests, Not National Plans, Shape Physician Workforce in the United States.” Family Medicine, vol. 52, no. 8, 2020, pp. 551–556. Available at https://pubmed.ncbi.nlm.nih.gov/32672833/. Accessed March 8, 2022.
Aizenberg, D.J., and L.S. Logio. “The Graduate Medical Education (GME) Gold Rush: GME Slots and Funding as a Financial Asset.” Academic Medicine, vol. 95, no. 4, April 2020, pp. 503–505. Available at https://journals.lww.com/academicmedicine/Fulltext/2020/04000/The_Graduate_Medical_Education__GME__Gold_Rush_.13.aspx?context=FeaturedArticles&collectionId=8.
Rittenhouse, D.R., A.S. Ament, and K. Grumbach. “Sponsoring Institution Interests, Not National Plans, Shape Physician Workforce in the United States.” Family Medicine, vol. 52, no. 8, 2020, pp. 551–556. Available at https://journals.stfm.org/familymedicine/2020/september/rittenhouse-2020-0088/.
Ahmed, H., and J B. Carmody. “On the Looming Physician Shortage and Strategic Expansion of Graduate Medical Education.” Cureus, vol. 12, no. 7, 2020, pp. e9216. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7430533/.
Albanese, A.P., E.T. Bope, K.M. Sanders, and M. Bowman. “The VA MISSION Act of 2018: A Potential Game Changer for Rural GME Expansion and Veteran Health Care.” Journal of Rural Health: Official Journal of the American Rural Health Association and the National Rural Health Care Association, vol. 36, no. 1, 2020, pp. 133–136. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6973037/.
Heisler, Elayne J., Sidath Viranga Panangala, Bryce H.P. Mendez, Marco A. Villagrana, and Alison Mitchell. “Federal Support for Graduate Medical Education: An Overview.” Washington, DC: Congressional Research Service, 2018. Available at https://fas.org/sgp/crs/misc/R44376.pdf. Accessed June 2, 2020.
Government Accountability Office. “HHS Needs Better Information to Comprehensively Evaluate Graduate Medical Education Funding.” Washington, DC: Government Accountability Office, 2018. Available at https://www.gao.gov/products/GAO-18-240. Accessed June 2, 2020.
Wynn, B. “Opening the ‘Black Box’ of GME Costs and Benefits: A Conceptual Model and a Call for Systematic Studies.” Journal of Graduate Medical Education, vol. 7, no. 1, March 2015, pp. 125–127. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4507905/pdf/i1949-8357-7-1-125.pdf. Accessed June 2, 2020.
Eden, J., D. Berwick, and G. Wilensky. Graduate Medical Education That Meets the Nation's Health Needs. Chicago, IL: National Academies Press, 2014: https://www.ncbi.nlm.nih.gov/books/NBK248027/. Accessed June 2, 2020.
Chang, B.K., and J.L. Brannen. “The Veterans Access, Choice, and Accountability Act of 2014: Examining Graduate Medical Education Enhancement in the Department of Veterans Affairs.” Academic Medicine, vol. 90, no. 9, 2015, pp. 1196–1198. Available at https://journals.lww.com/academicmedicine/fulltext/2015/09000/The_Veterans_Access,_Choice,_and_Accountability.13.aspx. Accessed June 2, 2020.
The National Academies of Sciences hosted a workshop in 2017 on the need to measure, track, and report GME outcomes. One of the findings of the workshop was that GME programs in their current form lack a shared understanding of what they should accomplish and operate independently of one another. Currently, no national mechanism exists for comprehensive assessments of whether GME programs accomplish their goals. Workshop participants discussed the value of measuring GME based on patient outcomes and community outcomes as well as how previous attempts to measure GME outcomes focused on metrics that were measurable but not important. Ultimately, the participants came up with seven key themes that had emerged during the workshop discussions, including the idea that measuring and reporting GME outcomes is important to justify public (Medicaid) funding.
Martin, P., M. Zindel, and S. Nass. “Graduate Medical Education Outcomes and Metrics: Proceedings of a Workshop.” Chicago, IL: National Academies Press, 2018. Available at https://www.nap.edu/download/25003#. Accessed May 27, 2020.
In this study, researchers produced a scoring tool that helped to predict whether physicians who completed their graduate medical education in an institution in Michigan would remain in Michigan after completing their training. Additional predictive variables in the study included being born in Michigan, competing medical school or obtaining a bachelor’s degree in Michigan, and completing a primary care residency. Their analysis showed that completing graduate medical education in Michigan was predictive of remaining in Michigan to practice medicine. The findings of this study support the theory that having ties to a state could influence a physician’s decision to remain and practice medicine after completing their training.
Koehler, T., J. Goodfellow, A. Davis, J. Spybrook, and J. van Schagen. “Predicting In-State Workforce Retention After Graduate Medical Education Training.” Journal of Graduate Medical Education, vol. 9, no. 1, February 2017, pp. 73–78. Available at https://www.jgme.org/doi/pdf/10.4300/JGME-D-16-00278.1. Accessed May 27, 2020.
Caverzagie, K.J., S.W. Lane, N. Sharma, J. Donnelly, J.R. Jaeger, H. Laird-Fick, J.P. Moriarty, et al. “Proposed Performance-Based Metrics for the Future Funding of Graduate Medical Education: Starting the Conversation.” Academic Medicine, vol. 93, no. 7, July 2018, pp. 1002–1013. Available at https://journals.lww.com/academicmedicine/Fulltext/2018/07000/Proposed_Performance_Based_Metrics_for_the_Future.20.aspx. Accessed June 2, 2020.
Chen, C., S. Petterson, R. Phillips, F. Mullan, A. Bazemore, and S. O’Donnell. “Toward Graduate Medical Education (GME) Accountability: Measuring the Outcomes of GME Institutions.” Academic Medicine, vol. 88, no. 9, September 2013, pp. 1267–1280. Available at https://journals.lww.com/academicmedicine/fulltext/2013/09000/Toward_Graduate_Medical_Education__GME_.31.aspx. Accessed June 2, 2020.
This article discusses California’s health workforce shortage and highlights lack of funding as a barrier to expanding graduate medical education (GME) and, ultimately, the physician workforce. It builds on the previous findings of the California Future Health Workforce Commission and explains the role of GME-naive hospitals in GME expansion. The authors identify the most pressing needs of GME-naive hospitals, including start-up funding and technical assistance. They also highlight examples of GME expansion in GME-naive hospitals in other states.
Rittenhouse, D.R., and A.S. Ament. “Expanding Graduate Medical Education in California: The Role of GME-Naive Hospitals.” CHCF Health Workforce Strategies for California Series. 2021. Available at https://www.chcf.org/wp-content/uploads/2021/06/WorkforceSeriesGMENaiveHospitals.pdf. Accessed March 8, 2022.
The California Future Health Workforce Commission compiled a final report as the culmination of two years of research into the future of the California health workforce. Its report examined the key issues facing California: that seven million Californians currently live in Health Professional Shortage Areas and that an upcoming wave of physician retirements is likely to exacerbate this crisis. The commission’s report included 27 recommendations, with 10 priority recommendations, for increasing opportunities for Californians in the health professions, expanding training and education in California, and increasing the capacity and retention of health care workers. One of the priority recommendations was to expand the number of primary care physician and psychiatry residency positions in California, with a goal of training an additional 1,872 primary care physicians and 2,202 psychiatrists by 2030.
California Future Health Workforce Commission. “Meeting the Demand for Health: Final Report of the California Future Health Workforce Commission.” February 2019. Available at https://futurehealthworkforce.org/wp-content/uploads/2019/03/MeetingDemandForHealthFinalReportCFHWC.pdf. Accessed May 27, 2020.
This article discusses the six teaching health centers in California, and their efforts to increase the number of primary care physicians in the state, especially in underserved areas. These teaching health centers are funded by grants from the Health Resources and Services Administration, but the future of this funding is uncertain. This analysis found that teaching health centers in California attract more applicants than they can admit, pointing to a need for increased training capacity. The analysis also found that most graduates of these programs continue to practice in underserved areas but may relocate to different geographic areas upon completion of their training.
Coffman, J., M. Fix, and K. Himmerick. “Preparing Physicians to Care for Underserved Patients: A Look at California's Teaching Health Centers.” Oakland, CA: California Health Care Foundation, 2016. Available at https://www.chcf.org/publication/preparing-physicians-to-care-for-underserved-patients-a-look-at-californias-teaching-health-centers/. Accessed June 2, 2020.
Weisbeck, K., A. Allard, K. Manko, M.M. Ford, and L. Cohen. “Primary Care Access in California and Disparities Across Major Cities.” New York, NY: Primary Care Development Corporation, 2020. Available at https://www.pcdc.org/wp-content/uploads/Points-on-Care-_-Issue-4-_-CA.pdf.
This policy brief looks at funding issues surrounding Rural Training Track (RTT) GME programs. A survey of RTT program directors and administrations found that RTT programs are often more responsible for program budget deficits than urban programs. The survey also found that these programs rely heavily on program administrators who donate their time to the program without compensation and on program directors who receive little compensation for the time they spend doing administrative work. The long-term viability of these RTT programs may be impacted by unstable funding arrangements.
Patterson D.G., D. Schmitz, R. Longenecker, D. Squire, and S.M. Skillman. “Graduate Medical Education Financing: Sustaining Medical Education in Rural Places.” Seattle, WA: WWAMI Rural Health Research Center, University of Washington, May 2015. Available at http://depts.washington.edu/uwrhrc/uploads/RTT_Finances_PB.pdf. Accessed June 2, 2020.
This annotated bibliography from the Robert Graham Center is split into two sections. The first reviews the current state of rural health care and the second reviews graduate medical education (GME) financing. Section one includes rural health needs, the mortality gap between urban and rural settings, and factors that contribute to this divergence. Section two includes an overview of the current GME financing structure, its impact on training, specific training programs financing, financing of safety net health care systems, and loan repayment programs. New policies regarding the structure of financing and physician workforce (rural and urban) are reviewed as possible solutions to financing complications. The analysis presented demonstrates a critical need for a national strategy that addresses rural workforce shortages and innovative financing of rural health care systems that will improve the quality and value of the American health care system.
Khatib, D., A. Huffstetler, and A. Bazemore. “Addressing Rural Workforce Shortages and Healthcare Disparities: An Annotated Bibliography.” Washington, DC: Robert Graham Center, n.d. Available at https://www.graham-center.org/content/dam/rgc/documents/publications-reports/reports/RuralHealth-AnnotatedBibliography-COGME.pdf. Accessed May 27, 2020.
Hawes, E.M., E. Fraher, S. Crane, A. Weidner, H. Wittenberg, J. Pauwels, R. Longenecker, et al. “Rural Residency Training as a Strategy to Address Rural Health Disparities: Barriers to Expansion and Possible Solutions.” Journal of Graduate Medical Education, vol. 13, no. 4, 2021, pp. 461–465. Available at https://pubmed.ncbi.nlm.nih.gov/34434506/. Accessed March 8, 2022.
Lultschik, J.L., and C.J. Martin. “Preventive Medicine for Rural America: Why More Training Programs Must Be Here.” Journal of Public Health Management and Practice, vol. 27, suppl. 3, 2021, pp. S151–S154. Available at https://journals.lww.com/jphmp/Fulltext/2021/05001/Preventive_Medicine_for_Rural_America__Why_More.8.aspx. Accessed March 8, 2022.
Albanese, A.P., E.T. Bope, K.M. Sanders, and M. Bowman. “The VA MISSION Act of 2018: A Potential Game Changer for Rural GME Expansion and Veteran Health Care.” Journal of Rural Health: Official Journal of the American Rural Health Association and the National Rural Health Care Association, vol. 36, no. 1, 2020, pp. 133–136. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6973037/.
Bruksch-Meck, K., B. Crouse, G. Quinn, L. McCart, and K. Traxler. “Graduate Medical Education Initiatives to Develop the Physician Workforce in Rural Wisconsin.” Wisconsin Medical Journal, vol. 117, no. 5, 2018, pp. 201–207. Available at https://wmjonline.org/wp-content/uploads/2018/117/5/201.pdf. Accessed June 2, 2020.
Starting a new ACGME approved residency program can positively impact patient care, medical education, hospital operations, and the community as whole. This requires a significant amount of commitment, time, and preparation. The initial application and accreditation process should start early and requires a thorough understanding on the ACGME requirements. Building a new residency program involves collaboration among various stakeholders, starting with the teaching hospital, ACGME, and the Center of Medicare and Medicaid services (CMS). It is prudent to also consider the operational and logistical issues such as budget, faculty and administrative staff hire, faculty time for administrative duties, and educational space for faculty and residents. It is vital to recognize how the institution’s strengths and weaknesses match up to these requirements. A robust educational and clinical curriculum in line with ACGME’s core competencies and useful educational collaboration among various programs is critical for effective program. Recruiting and developing the appropriate faculty members is another important aspect for a successful program. The final challenge is recruiting residents that will fit well into the new residency program. Lastly, we discuss the challenges and tips to mitigate the risks of disappointment in the process of starting and creating a flagship residency program.
Goodbred, A., R. Snyder, J. Sweeny, C. Marchionni, B. Bhatt, G. Domer, A. Davis, S. Yaich, J. Orlando, J. Dalkiewicz, M. Geary, V. Yellapu and P. Kaur. “Starting New Accreditation Council for Graduate Medical Education (ACGME) Residency Programs in a Teaching Hospital.” Contemporary Topics in Graduate Medical Education [Working Title], vol. 2, 2020, doi:10.5772/intechopen.73480. Available at https://www.intechopen.com/online-first/starting-new-accreditation-council-for-graduate-medical-education-acgme-residency-programs-in-a-teac. Accessed February 15, 2021.
This article begins with a discussion of the current state of graduate medical education (GME) funding in the United States as well as the medical education system in Georgia. The authors then describe the steps that Georgia took to expand GME, including establishing new residency programs in the state, noting that residents who train in Georgia are more likely to remain in the state throughout their careers. The article outlined the costs and infrastructure needs associated with transitioning from a community hospital to a teaching hospital and how funding from the state of Georgia was dispersed to create about 400 new residency positions beginning in 2013. The article concludes with a discussion of the lessons learned and challenges faced by the new GME programs.
Nuss, M., B. Robinson, and P. Buckley. “A Statewide Strategy for Expanding Graduate Medical Education by Establishing New Teaching Hospitals and Residency Programs.” Academic Medicine, vol. 90, no. 9, September 2015, pp. 1264–1268. Available at https://journals.lww.com/academicmedicine/fulltext/2015/09000/A_Statewide_Strategy_for_Expanding_Graduate.27.aspx. Accessed May 27, 2020.
This article was about the GME Initiative- a grassroots group made up of medical educators, advocates, and leaders - and their work to reform graduate medical education. The GME Initiative workgroup strives to “connect the dots” between the intent of GME reform strategies and the actual results. The GME Initiative hosted its first summit focused on states in 2017, and representatives from 33 states attended. Interested parties can contact the GME Initiative leaders for more information about how to get involved.
Davis A., and M. Singh. “The GME Initiative” And GME In States.” Annals of Family Medicine, vol. 16, no. 5, September 2018, pp. 468-469. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6130997/. Accessed June 5, 2020.
Newton, W., N. Wouk, and J. Spero. “Improving the Return on Investment of Graduate Medical Education in North Carolina.” North Carolina Medical Journal, vol. 77, no. 2, March 2016, pp. 121–127. Available at https://www.ncmedicaljournal.com/content/77/2/121.long. Accessed November 4, 2020.
New Mexico Human Services Department. “GME Expansion in NM: 5-Year Strategic Plan.” Santa Fe, NM: New Mexico Human Services Department, 2019. Available at https://www.hsd.state.nm.us/uploads/files/GME%20Expansion/GMEStrategicPlanRFA2019_11_29_ACS%20(002).pdf. Accessed June 2, 2020.
Ashkin, E., W. Newton, B. Toomey, R. Lingley, and C. Page. “Cost of Incremental Expansion of an Existing Family Medicine Residency Program.” Society of Teachers of Family Medicine, vol. 49, no. 7, 2017, pp. 544–547. Available at https://www.stfm.org/FamilyMedicine/Vol49Issue7/Ashkin544. Accessed May 27, 2020.
Fraher, E., and J. Spero. “State-Based Approaches to Reforming Medicaid-Funded Graduate Medical Education.” Chapel Hill, NC: Carolina Health Workforce Research Center, 2017. Available at https://www.shepscenter.unc.edu/wp-content/uploads/2017/01/GMEI-States-Initiatives-Summit-1_25_17FINAL.pdf. Accessed June 2, 2020.
Kornegay, D. “GME IN GEORGIA: Growth, Funding, and Sustainability.” Augusta, GA: Augusta University, 2016. Available at https://www.augusta.edu/ahec/documents/gme_white_paper.pdf. Accessed June 2, 2020.
Henderson, T. “Medicaid Graduate Medical Education Payments: A 50-State Survey.” Washington, DC: Association of American Medical Colleges, 2016. Available at https://store.aamc.org/downloadable/download/sample/sample_id/246/. Accessed June 2, 2020.
Texas Higher Education Coordinating Board. “An Assessment of Opportunities for Graduates of Texas Medical Schools to Enter Graduate Medical Education in Texas.” Austin, TX: Texas Higher Education Coordinating Board, 2016. Available at http://www.thecb.state.tx.us/DocID/PDF/8649.PDF. Accessed June 2, 2020.
Nuss, M., and P. Buckley. “Georgia's Innovative Response to GME Expansion.” Journal of the Medical Association of Georgia, vol. 104, 2015, pp. 10–11. Available at https://www.ncbi.nlm.nih.gov/pubmed/26492741. Accessed June 2, 2020.
Kaufman, A., and C. Alfero. “A State-Based Strategy for Expanding Primary Care Residency.” Health Affairs Blog, 2015. Available at https://www.healthaffairs.org/do/10.1377/hblog20150731.049707/full/. Accessed June 2, 2020.
Spero, J.C., E.P. Fraher, T.C. Ricketts, and P.H. Rockey. “GME in the United States: A Review of State Initiatives.” Chapel Hill, NC: Center for Health Services Research, 2013. Available at https://www.shepscenter.unc.edu/wp-content/uploads/2013/09/GMEstateReview_Sept2013.pdf. Accessed June 2, 2020.
Blewett, L.A., and V. Weslowski. “New Roles for States In Financing Graduate Medical Education: Minnesota’s Trust Fund.” Health Affairs, vol. 19, no. 1, 2000. Available at https://www.healthaffairs.org/doi/full/10.1377/hlthaff.19.1.248. Accessed June 2, 2020.
Ohio Association of Community Health Centers. “Ohio Primary Care Workforce Initiative (OPCWI) User Manual.” Columbus, OH: Ohio Association of Community Health Centers, n.d. Available at https://cdn.ymaws.com/www.ohiochc.org/resource/resmgr/opcwi/OPCWI_User_Manual_Webpage.pdf. Accessed June 2, 2020.
In this article, the authors discuss the impetus for Congress’s authorization of the Teaching Health Center GME program as part of the Affordable Care Act and assess the cost for a Teaching Health Center to provide GME residency training. The Teaching Health Center GME program was designed to increase the number of primary care physicians and dentists trained in community-based settings with the goal of bolstering long-term clinical capacity in those settings. It provides a set amount per resident per year to the Teaching Health Centers that participate, dependent on Congressional appropriations. The initial amount appropriated was $150,000 per resident. The authors analyzed to determine whether this amount reflects the costs incurred by a Teaching Health Center and found it to be reasonably reflective of the actual cost.
Regenstein, M., K. Nocella, M.M. Jewers, and F. Mullan. “The Cost of Residency Training in Teaching Health Centers.” The New England Journal of Medicine, vol. 375, no. 7, August 18, 2016, pp. 612–614. Available at https://www.nejm.org/doi/10.1056/NEJMp1607866. Accessed May 27, 2020.
Garces de Marcilla, J., K. Abreu, L. Peterson, and S. Weinman. “Teaching Hospitals and FQHCs Can Partner to Alleviate Community Healthcare Provider Shortages and Reduce Training Costs.” FQHC.org Blog, 2017. Available at https://www.fqhc.org/blog/2017/4/27/unusual-hospital-fqhc-partnerships-address-payment-and-access-issues. Accessed June 2, 2020.
Coffman, J., M. Fix, and K. Himmerick. “Preparing Physicians to Care for Underserved Patients: A Look at California's Teaching Health Centers.” Oakland, CA: California Health Care Foundation, 2016. Available at https://www.chcf.org/publication/preparing-physicians-to-care-for-underserved-patients-a-look-at-californias-teaching-health-centers/. Accessed June 2, 2020.
Rieselbach, R., P. Shin, G. Nycz, K. Pereira, N. Short, E. McConnell, and K. Schmader. “Mega Teaching Health Centers: A New Model to Power CHCs.” Health Affairs Blog, 2016. Available at https://www.healthaffairs.org/do/10.1377/hblog20161013.057067/full/. Accessed June 2, 2020.
Chen C., F. Chen, and F. Mullan. “Teaching Health Centers: A New Paradigm in Graduate Medical Education.” Academic Medicine, vol. 87, no. 12, 2012, pp. 1752–1756. Available at https://pubmed.ncbi.nlm.nih.gov/23095929/. Accessed June 2, 2020.
Advisory Board
- Anthony Albanese, MD, FACP, DFASAM Director, MISSION Act, RIFDI & GME Expansion
VA Office of Academic Affiliations (OAA) - Lupe Alonzo-Diaz, MA
President/CEO
Physicians for a Healthy California - Theresa Azevedo, MPA
Associate Institutional Director and DIO
Kaiser Permanente Northern California - Peter Broderick, MD, MEd
Director of Undergraduate Medical Education, Valley Region
Sutter Health - Janet Coffman
Professor of Health Policy and Family and Community Medicine
University of California, San Francisco - J. Craig Collins, MD, MBA
DIO
Kaiser Permanente Southern California - David Connett, DO
Vice Dean
Western University of Health Sciences – College of Osteopathic Medicine - James Cruz, MD
Senior Medical Director
Blue Shield of CA Promise Health Plan - Jeremy Fish, MD
Program Director, Family Medicine Residency
John Muir Health - Hector Flores, MD
Co-Director, Family Medicine Residency Program
White Memorial Medical Center - C. Freeman, MD, MBA
Adult and Geriatric Psychiatrist
Los Angeles, CA - Dean Germano, MHSC
CEO
Shasta Community Health Center - Daniel Giang, MD
Associate Dean, GME
Loma Linda University School of Medicine - Kevin Grumbach, MD
Chair, Family and Community Medicine
University of California, San Francisco
- Caryn Rizell
Acting Deputy Director
Office of Statewide Health Planning and Development - William Henning, DO
Member
California Healthcare Workforce Policy Commission - Robert McCarron, DO
Vice Chair of Education and Integrated Care, Department of Psychiatry and Human Behavior
University of California, Irvine - Cathryn Nation, MD
Vice President – Health Services
University of California Office of the President - Kiki Nocella, MHA, PhD
Director
WIPFLi - Michelle Nuss, MD
Campus Associate Dean for GME
Augusta University/University of Georgia Medical Partnership - Richard Riemer, DO
Senior Associate Dean
Touro University California - Mark Servis, MD
Vice Dean for Medical Education
University of California, Davis - Stacey Silverman, PhD
Deputy Assistant Commissioner, Academic Quality
Texas Higher Education Coordinating Board - Mannat Singh, MPA
Director
The GME Initiative - Efrain Talamantes, MD, MBA
Medical Director
AltaMed Institute for Health Equity - Lori Weichenthal, MD, FACEP
Assistant Dean of GME and DIO
UCSF Fresno - Lori Winston, MD
DIO
Kaweah Delta Health Care District
Key Staff

Alexandra Ament
Independent Contractor



